Hip Pain Treatment
in Ryde, Isle of Wight
Hip pain can stop you in your tracks. Whether it is a nagging ache on the side of your hip, stiffness when you get up in the morning, pain in your groin when you walk, or discomfort that keeps you awake at night, it can affect everything from getting dressed to enjoying a walk.
Hip pain does not always come from the hip itself. It can be referred from the lower back, the glutes, or the surrounding soft tissue. Getting to the root of it matters. That is what the initial assessment is for.
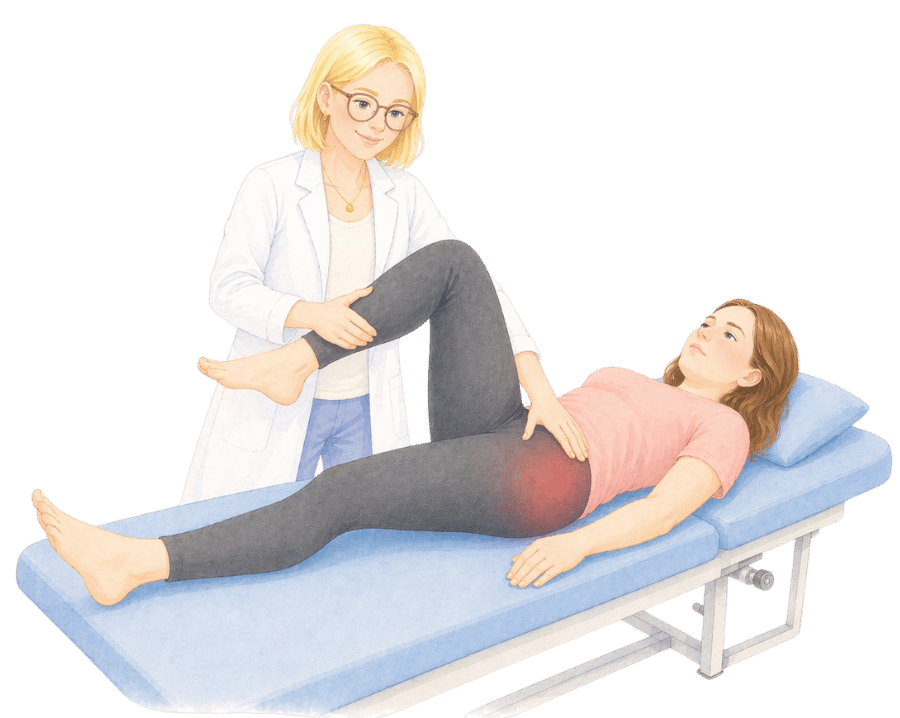
When should you get hip pain checked urgently?
Most hip pain is not a medical emergency. But some presentations need prompt attention. Contact your GP or 111 as a priority if you have:
- Hip pain following a fall or significant impact, particularly if you cannot bear weight
- Severe hip pain with fever, feeling generally unwell, or hot swollen skin over the joint (possible infection)
- Sudden severe hip or groin pain with no clear cause
- Hip pain in a child that came on suddenly (seek same-day medical review)
- Known osteoporosis or long-term steroid use combined with sudden hip pain
- Unexplained weight loss alongside persistent hip pain
These presentations need medical assessment first. If none of these apply and your hip pain has built up gradually or follows activity, osteopathy may be able to help.
Start your Care Journey Today

What does hip pain feel like?
Hip pain presents differently from person to person. Some of the most common patterns Serena sees in practice include:
- Pain on the outside (lateral) of the hip. This often aches at rest, flares when walking, and can be worse lying on the affected side at night. It is commonly associated with gluteal tendinopathy or greater trochanteric pain syndrome.
- Pain deep in the groin or front of the hip. This may radiate into the thigh and feel worse when sitting for long periods, climbing stairs, or crossing your legs. Hip joint stiffness often presents this way.
- Stiffness in the morning. Hips that take a while to loosen up after sleep or rest, easing with gentle movement but returning after inactivity, are a familiar presentation.
- A general ache in the buttock or outer thigh. This can radiate from the lower back or be related to the piriformis muscle and the sciatic nerve pathway.
- Pain that started after increasing activity. Runners, cyclists, and people who have recently increased their walking often present with hip overuse patterns, particularly involving the hip flexors or glutes.
You may recognise one of these clearly, or your symptoms may be a mix. The assessment is designed to work it out.
What causes hip pain?
Hip pain has many possible causes, and the same symptoms can come from quite different sources. Some of the most common presentations Serena assesses include:
- Gluteal tendinopathy and greater trochanteric pain syndrome: Pain on the outside of the hip, often worse when lying on it or sitting with legs crossed. Caused by load or compression on the gluteal tendons, often triggered by sudden changes in activity levels.
- Hip joint stiffness and early osteoarthritis: Gradual stiffening, reduced range of movement, and a deep ache in the groin or front of the hip, particularly in people over 50. Movement tends to ease it temporarily; rest may stiffen it again.
- Piriformis syndrome: Deep buttock pain that can mimic or accompany sciatica. The piriformis muscle sits close to the sciatic nerve, and tightness or irritation can refer pain into the back of the hip and thigh.
- Hip flexor strain: Pain at the front of the hip, often following increased walking, cycling, or periods of prolonged sitting. The hip flexors can become overloaded with repetitive activity.
- Referred pain from the lower back: The lumbar spine and hip share nerve pathways. Pain that appears to come from the hip can sometimes originate in the lower back, particularly if there is also leg pain, numbness, or tingling.
- Bursitis: The bursae are small fluid-filled sacs that cushion the hip joint. When irritated, often alongside tendon problems, they can produce an aching, sensitive hip that is sore to pressure.
Getting the cause right shapes the management. That is a core part of what the initial assessment is for.
Hip pain and other areas
Hip pain does not always stay neatly within the hip joint. It is common for pain to refer from one area into another, and patients are often unsure where the problem is actually coming from.
The lower back and the hip share nerve pathways. Pain that presents in the hip, groin, or buttock can sometimes originate in the lumbar spine, particularly if there is also leg pain, tingling, or numbness. An assessment is the most reliable way to work out which area is driving which.
The knee and foot can also be affected by how the hip is loading and moving. Hip weakness, for example, can change how forces travel through the leg during walking, which can contribute to knee or foot symptoms. These connections matter when building a management plan.
This page focuses on hip-led presentations. If your main complaint is back pain, the back pain page covers that in more detail.
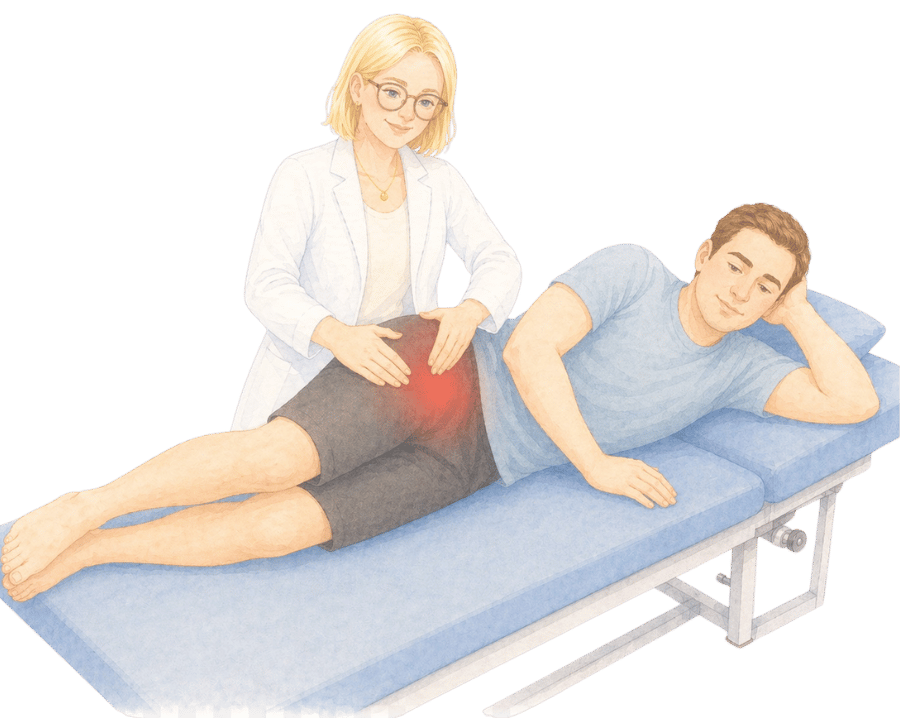
How can osteopathy help with hip pain?
Osteopathy does not offer a quick fix for every hip problem, and Serena will not tell you it does. What it can offer is a thorough assessment, a working explanation of what is happening, and a plan adapted to your situation.
For conditions such as gluteal tendinopathy and trochanteric pain, the evidence supports graduated loading as a key part of recovery. Serena draws on current pain science and rehabilitation principles, not just manual technique.
Sports massage may also be useful alongside osteopathy for hip presentations involving soft tissue tightness, overuse, or post-activity soreness.
Our approach to hip pain:
- Reduce discomfort in the surrounding muscles, tendons, and soft tissue
- Improve joint mobility where restriction is contributing to your symptoms
- Identify any loading or movement patterns that may be aggravating the problem
- Give you a clear self-management plan so you are not dependent on repeat appointments
- Advise you honestly about whether further investigation or referral would be appropriate
What to expect in appointments when you have a chronic condition
Your first appointment at Lind Street Osteopathy lasts 60 minutes. Hip pain can have a number of causes — from the joint itself to the surrounding muscles, the lower back or the way you move and load your body day to day. Serena will take time to understand your situation fully before recommending any treatment. Here is what to expect:
- Case history: Serena will ask about your hip pain: where exactly you feel it, whether it is deep in the joint, in the groin, on the outer hip or down into the thigh, and what makes it better or worse. She will also ask about your activity levels, occupation, any history of injury or arthritis, and how the pain is affecting your daily life, such as walking, stairs or getting up from a chair.
- Examination: It will typically include hands-on assessment of the hip joint, surrounding muscles, lower back and sacroiliac joints, as these areas work closely together and pain in one often reflects strain in another.
- Examination: Serena will discuss whether osteopathic treatment is appropriate for you, and whether any imaging or onward referral would be worth considering.
- Examination: Hip pain treatment may include soft tissue work to release tight muscles around the hip and pelvis, joint articulation to improve mobility, and techniques to address any contributing stiffness in the lower back or sacroiliac joints. Treatment is always adapted to your comfort and to the nature of your condition.
- Home advice: You will leave with practical guidance tailored to your situation. This might include movement or stretching recommendations, advice on activity modification, tips on positions to avoid or support, and guidance on how to keep the hip and surrounding muscles working well between sessions.
Follow-up appointments for chronic conditions are 45 minutes. Some patients benefit from a short initial course of treatment; others find occasional sessions over time more useful. This will be discussed openly.
Hip pain self-help:
What you can do now
While you are deciding what to do, or alongside any treatment you receive, there are things that may help with many types of hip pain.

Keep moving, gently
Rest is rarely the best answer for hip pain, and complete rest can sometimes make things worse. Short, regular walks at a comfortable pace tend to be more useful than alternating between overactivity and prolonged rest.

Gentle glute strengthening
Building strength in the gluteal muscles is one of the most consistently supported approaches for lateral hip pain. Simple exercises such as side-lying leg raises or single-leg standing (if comfortable) can be a useful starting point.

Manage how you load the hip
If pain on the outside of the hip is worse after sitting with legs crossed or lying on the affected side, adjusting those habits can reduce irritation. For lateral hip pain, sitting with feet flat and hips level is generally more comfortable than sitting with one knee higher.
These suggestions are general and may not apply to every presentation. Serena will give you specific guidance based on your individual assessment.

Stairs and slopes
Going upstairs can load the hip in ways that aggravate certain conditions. Slowing down and using a handrail where helpful can reduce flare-ups while things settle.

Avoid sudden increases in activity
If your hip pain followed a sharp increase in walking, running, or exercise, reducing intensity temporarily while gradually rebuilding tolerance often helps more than stopping altogether.
These suggestions are general and may not apply to every presentation. Serena will give you specific guidance based on your individual assessment.
Frequently asked questions
about hip pain
We know starting something new can bring up a few questions — especially if it’s your first time seeing an osteopath. Below you’ll find answers to some of the most common things people ask us. If you’re still unsure about anything, don’t hesitate to get in touch — we’re here to help.
Hip pain when walking is one of the most common patterns Serena sees. The cause varies, but frequent reasons include gluteal tendinopathy (outside of the hip), hip joint stiffness, referred pain from the lower back, or a hip flexor overuse pattern. A thorough assessment is the most reliable way to work out which is at play
Not quite, though the two often occur together. Bursitis refers to irritation of the bursa, a small fluid-filled cushion near the hip, while glute tendinopathy involves the gluteal tendons themselves. The symptoms can feel very similar: pain on the outside of the hip, worse with prolonged walking or lying on the affected side. Management overlaps but is not identical, which is why the distinction matters.
Yes. The lumbar spine and the hip share nerve pathways, and problems in the lower back can refer pain into the hip, groin, or buttock. If you have hip pain alongside back pain, leg pain, or any tingling or numbness, it is worth assessing both areas to understand where the primary issue lies.
If your hip pain has been present for more than a week or two without improving, is affecting your sleep or daily activities, or followed a change in activity levels, it is worth getting it assessed. Many hip conditions respond well to the right management. The sooner you understand what is going on, the better placed you are to address it. Serena's clinic is based in Ryde and sees patients from across the Isle of Wight.
Book an appointment in Ryde
If you would like to talk through whether this service is right for you, or if you are ready to book, Serena would be happy to hear from you.
- 07528 966206
- lindstreetosteopathy.co.uk
-
Lind Street Osteopathy
17 Lind Street, Ryde, Isle of Wight, PO33 2NQ
Lind Street Osteopathy is based in Ryde on the Isle of Wight. Serena sees patients from across Ryde and the wider island, including Bembridge, Brading, Seaview, Shanklin, Sandown, and Newport.
The clinic is situated in a Victorian townhouse in the heart of Ryde, at 17 Lind Street, Ryde, Isle of Wight, PO33 2NQ. It is easily reached from most parts of the island.