Fibromyalgia: Why Your Pain Isn’t Imaginary and What You Can Do About It
Serena Johnson
April 8, 2026
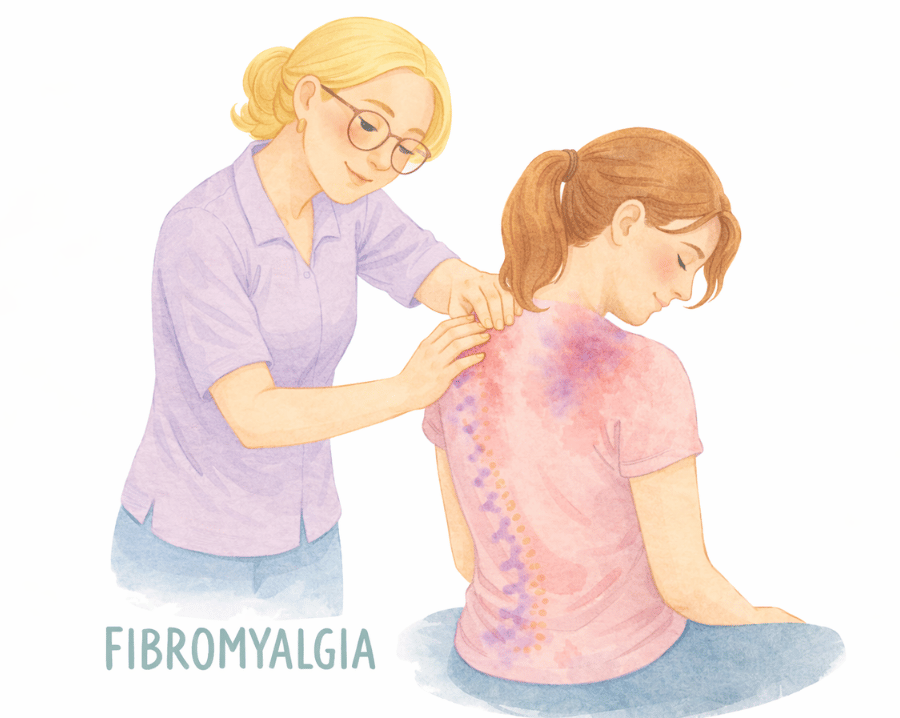

If you’ve been living with widespread pain, fatigue, poor sleep, and “brain fog” that doesn’t seem to have a clear cause, you may have come across Fibromyalgia.
This is something we commonly see in clinic here on the Isle of Wight, particularly among women dealing with long-term or fluctuating pain.
Fibromyalgia can feel frustrating and isolating, especially when test results appear normal. But the symptoms are very real, and understanding what’s happening in the body is the first step toward managing them more effectively.
What Is Fibromyalgia?
Fibromyalgia is a chronic condition characterised by:
- Widespread musculoskeletal pain
- Ongoing fatigue
- Sleep disturbances
- Cognitive difficulties often described as “fibro fog”
- Sensitivity to touch, pressure, temperature, or noise
- Digestive issues such as IBS in some people
Unlike conditions caused by visible tissue damage, fibromyalgia is believed to involve how the nervous system processes pain. This means the body becomes more sensitive to signals that would not normally be painful.
Why Does Fibromyalgia Happen?
There is no single cause of fibromyalgia. Instead, it is thought to develop from a combination of factors, including:
1. Nervous system sensitivity
The central nervous system becomes more reactive to pain signals, a process known as central sensitisation. This can lead to pain being felt more intensely and more widely.
2. Genetics
Fibromyalgia can run in families, suggesting some people may have a genetic predisposition.
3. Triggers
Symptoms may begin or worsen after:
- Physical injury or trauma
- Illness or infection
- Significant emotional stress
- Long-term stress or life changes
4. Ongoing stress and fatigue cycles
Stress, poor sleep, and pain can reinforce each other, making symptoms more persistent over time.
Our
Newsletters
Sign up to receive simple tips, updates, and insights from the clinic — designed to help you feel better, move more freely, and take care of your health.
Common Symptoms of Fibromyalgia
Symptoms can vary from person to person and may fluctuate over time. Common features include:
Widespread Pain
Pain is often described as aching, burning, or throbbing, and can affect multiple areas of the body.
Fatigue
This is not ordinary tiredness. It can feel like a deep exhaustion that doesn’t improve with rest.
Fibro Fog
Difficulty concentrating, memory issues, and reduced mental clarity.
Sleep Disturbances
Many people struggle to fall asleep, stay asleep, or feel refreshed in the morning.
Increased Sensitivity
Heightened sensitivity to:
- Touch
- Pressure
- Temperature
- Light or noise
Digestive Symptoms
Some people also experience IBS-type symptoms such as bloating, abdominal pain, or changes in bowel habits.
Why Symptoms Can Fluctuate
Fibromyalgia symptoms often come and go. Many people notice flare-ups triggered by:
- Stress
- Poor sleep
- Overexertion
- Cold or damp weather
Periods of improvement may be followed by times when symptoms increase again. This variability is a normal part of the condition.
How Is Fibromyalgia Diagnosed?
There is no single test for fibromyalgia. Diagnosis is based on symptoms, medical history, and ruling out other conditions.
Healthcare professionals now use symptom-based criteria that consider:
- Widespread pain across the body
- Symptom severity (fatigue, sleep, cognitive issues)
- Duration and pattern of symptoms
Because symptoms overlap with other conditions, it’s important that fibromyalgia is diagnosed carefully to ensure appropriate support.
Can Fibromyalgia Be Cured?
There is currently no cure for fibromyalgia. However, many people are able to manage their symptoms and improve their quality of life through a combination of approaches.
The goal is not necessarily to eliminate symptoms completely, but to:
- Reduce flare-ups
- Improve function
- Support the nervous system
- Build confidence in movement and daily activity
How Osteopathy Can Help Fibromyalgia
Osteopathy takes a holistic approach, focusing on how the body moves and functions as a whole.
While osteopathy does not “cure” fibromyalgia, it can help support the body in several ways:
- Reducing muscle tension and physical strain
- Improving mobility in joints and soft tissues
- Supporting circulation and relaxation
- Helping the body move more efficiently
- Providing guidance on posture and daily movement habits
- Offering reassurance and education about pain
Many people with fibromyalgia benefit from gentle, tailored treatment that is adapted to their sensitivity levels on the day.
What Helps Manage Fibromyalgia Symptoms?
A combination approach tends to work best. This may include:
- Gentle, regular movement (within tolerance)
- Pacing activities rather than overdoing it
- Prioritising sleep quality
- Stress management techniques such as breathing or mindfulness
- Education about pain and the nervous system
- Support from healthcare professionals
Consistency and gradual progress are often more effective than pushing through symptoms.
Living with Fibromyalgia
Living with fibromyalgia can be challenging, particularly when symptoms are unpredictable. However, many people find that with the right support, they can regain a sense of control over their condition.
Understanding your triggers, learning how your body responds, and working with professionals who recognise the complexity of chronic pain can make a significant difference.
When to Seek Help
If you are experiencing ongoing widespread pain, fatigue, or other symptoms that are affecting your daily life, it’s important to seek assessment and support.
Early guidance can help rule out other conditions and provide clarity on the best way forward.
Frequently Asked Questions About Fibromyalgia
Is fibromyalgia a real condition?
Yes. Fibromyalgia is a recognised chronic condition involving how the nervous system processes pain. The symptoms are real and can significantly impact daily life.
Why do tests come back normal?
Fibromyalgia does not typically show up on standard blood tests or imaging because it is related to pain processing rather than structural damage.
Does fibromyalgia get worse over time?
It varies. Symptoms can fluctuate, and with the right management strategies, many people are able to stabilise or improve their condition.
Can osteopathy help fibromyalgia?
Osteopathy can help support mobility, reduce tension, and improve comfort, alongside providing advice tailored to your body and symptoms.
What makes fibromyalgia flare up?
Common triggers include stress, poor sleep, overexertion, illness, and sometimes environmental factors like cold weather.
What this means for you
Fibromyalgia is a complex condition, but understanding it can make it feel much more manageable. With the right combination of support, movement, and lifestyle strategies, many people are able to improve their symptoms and quality of life.
If you’re living with fibromyalgia on the Isle of Wight and would like support in managing your symptoms, a personalised approach can help you move more comfortably and confidently again.